সকল ধরনের প্যাথলজিক্যাল টেস্ট করানো হয় 01797522136
ভূমিকা
বর্তমান যুগে সঠিক রোগ নির্ণয়ের জন্য প্যাথলজিক্যাল টেস্ট অত্যন্ত গুরুত্বপূর্ণ। রোগ নির্ণয়, চিকিৎসা পরিকল্পনা, চিকিৎসার অগ্রগতি পর্যবেক্ষণ এবং রোগ প্রতিরোধ—সব ক্ষেত্রেই ল্যাবরেটরি পরীক্ষার ভূমিকা অপরিসীম। কিন্তু অনেক সময় উচ্চমূল্যের কারণে সাধারণ মানুষ প্রয়োজনীয় টেস্ট করাতে পারেন না। এই সমস্যা সমাধানের জন্য সরকার নির্ধারিত মূল্য তালিকা অনুসারে প্যাথলজিক্যাল টেস্ট করার উদ্যোগ অত্যন্ত গুরুত্বপূর্ণ।

HRTD Medical Institute, সেকশন-৬, ব্লক-খা, রোড-১, প্লট-১১, মেট্রোরেল পিলার-২৪৯, ফলপট্টি মসজিদ লেন, মিরপুর-১০, ঢাকা-১২১৬—এ অবস্থিত একটি বিশ্বস্ত ও সুনামধন্য প্রতিষ্ঠান, যেখানে সরকার নির্ধারিত মূল্যে সকল ধরনের প্যাথলজিক্যাল টেস্ট সম্পন্ন করা হয়। আমাদের লক্ষ্য হলো স্বল্প খরচে নির্ভুল ও মানসম্মত পরীক্ষার মাধ্যমে জনসাধারণকে স্বাস্থ্যসেবা প্রদান করা।
যোগাযোগ:
01797522136
01987073965
01784572173
আমাদের অঙ্গীকার
HRTD Medical Institute সবসময় স্বচ্ছতা, নির্ভুলতা এবং সেবার মান বজায় রেখে কাজ করে। আমরা প্রতিশ্রুতিবদ্ধ:
- সরকার নির্ধারিত মূল্যে টেস্ট প্রদান
- নির্ভুল ও দ্রুত রিপোর্ট সরবরাহ
- আধুনিক যন্ত্রপাতি ব্যবহার
- দক্ষ ও প্রশিক্ষিত টেকনোলজিস্ট দ্বারা পরীক্ষা সম্পন্ন
- রোগীবান্ধব পরিবেশ নিশ্চিত করা
আমাদের বিশ্বাস, স্বাস্থ্যসেবা কোনো বিলাসিতা নয়—এটি সবার মৌলিক অধিকার।

কেন সরকার নির্ধারিত মূল্যে টেস্ট গুরুত্বপূর্ণ?
সরকার নির্ধারিত মূল্য তালিকা অনুসরণ করার ফলে:
১. রোগীরা অতিরিক্ত অর্থ প্রদান থেকে রক্ষা পান
২. সব শ্রেণির মানুষ সমানভাবে চিকিৎসা সুবিধা পান
৩. স্বাস্থ্যখাতে স্বচ্ছতা বজায় থাকে
৪. চিকিৎসা ব্যবস্থায় আস্থা বৃদ্ধি পায়
৫. নিম্ন ও মধ্যবিত্ত পরিবারের আর্থিক চাপ কমে
HRTD Medical Institute এই নীতিকে সম্পূর্ণভাবে অনুসরণ করে থাকে।

আমাদের প্যাথলজিক্যাল সেবাসমূহ
আমাদের প্রতিষ্ঠানে সরকার নির্ধারিত মূল্যে নিম্নোক্ত সকল ধরনের প্যাথলজিক্যাল টেস্ট করা হয়:
১. হেমাটোলজি বিভাগ
রক্ত সম্পর্কিত বিভিন্ন রোগ নির্ণয়ে হেমাটোলজি টেস্ট অত্যন্ত গুরুত্বপূর্ণ।
আমাদের সেবাসমূহ:
Complete Blood Count (CBC)
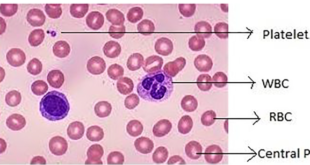
A Complete Blood Count (CBC) is a common, fundamental blood test that measures the cells circulating in the blood, including red blood cells (RBCs), white blood cells (WBCs), and platelets. It evaluates overall health, detects infections, anemia, and leukemia, and helps monitor disease, typically requiring a small venous blood sample.
Key Components Measured
- Red Blood Cells (RBCs): Measures oxygen-carrying cells, including hemoglobin (oxygen protein) and hematocrit (percentage of blood composed of RBCs).
- White Blood Cells (WBCs): Measures the cells that fight infection; a differential may be included to break down the five types of white cells.
- Platelets: Measures the cells responsible for blood clotting.
- Mean Corpuscular Volume (MCV): Measures the average size of red blood cells.
Common Reasons for a CBC
- Routine Health Checkup: Part of a standard physical.
- Diagnosing Illness: Identifying causes of fatigue, weakness, bruising, or fever.
- Monitoring Conditions: Tracking blood diseases, infections, or effects of treatments like chemotherapy.
Normal Ranges (General Guidance)
Note: Reference ranges vary by laboratory.
- WBC: 4,500 to 11,000 cells/mcL
- RBC: 4.5–5.9 million cells/mcL (Men); 4.1–5.1 million cells/mcL (Women)
- Hemoglobin: 14–17.5 gm/dL (Men); 12.3–15.3 gm/dL (Women)
- Hematocrit: 41.5%–50.4% (Men); 35.9%–44.6% (Women)
- Platelets: 150,000 to 450,000 platelets/mcL
ESR
An Erythrocyte Sedimentation Rate (ESR) test measures how quickly red blood cells sink to the bottom of a test tube, acting as a non-specific indicator of inflammation, infection, or cancer in the body. Faster sinking times (higher ESR) indicate elevated inflammation, with results measured in millimeters per hour.

Key Details About the ESR Test:
- Purpose: It helps diagnose or monitor inflammatory conditions like autoimmune diseases, infections, or certain cancers, but cannot identify the specific cause.
- Procedure: A blood sample is placed in a tube, and the distance the red blood cells fall in one hour is measured.
- Normal Values: Generally, 0–15
for men under 50, and 0–20
for women under 50; higher ranges are common in elderly patients.
- High ESR Results: Values above 100
may suggest significant underlying, active disease.
- Limitations: The test is non-specific; an elevated ESR does not identify a specific disease, and a normal ESR does not rule out all diseases.
Blood Group & Rh Typing
Blood grouping (ABO) and Rh typing determine the presence of specific antigens on red blood cells, resulting in 8 main types (A+, A-, B+, B-, O+, O-, AB+, AB-). ABO is based on A/B antigens, while Rh typing identifies the presence (+) or absence (-) of the RhD protein. This, crucial for safe blood transfusions and pregnancy, involves a simple blood test.
Key Aspects of Blood Grouping and Rh Typing
- ABO System: Classifies blood into A, B, AB, or O based on surface antigens.
- Type A: A antigens.
- Type B: B antigens.
- Type AB: Both A and B antigens.
- Type O: Neither A nor B antigens.
- Rh System: Determines if blood is positive (+) or negative (-) based on the presence of the RhD antigen.
- Rh-positive (+): RhD antigen is present.
- Rh-negative (-): RhD antigen is absent.
- Importance:
- Transfusion Safety: Ensures compatibility to avoid severe immune reactions.
- Pregnancy: Crucial for identifying Rh-incompatibility, where an Rh-negative mother carries an Rh-positive fetus, potentially leading to hemolytic disease of the newborn.
- Emergency Situations: O-negative blood is often used as the universal donor in emergencies.
- Procedure: A laboratory technician mixes a blood sample with antibodies (anti-A, anti-B, and anti-Rh) and observes for agglutination (clumping) to determine the blood type.
Common Blood Types (U.S.)
- Most Common: O positive (O+).
- Least Common: AB negative (AB-).
Rh-Negative Considerations
Rh-negative individuals can develop antibodies to the Rh antigen if exposed to Rh-positive blood (e.g., via transfusion or pregnancy), which can cause complications in future exposures.
Peripheral Blood Film
A peripheral blood film (PBF) or smear is a laboratory test where a thin layer of blood is spread on a glass slide, stained, and examined microscopically to analyze the morphology, number, and size of red cells, white cells, and platelets. It is a critical diagnostic tool for identifying blood diseases like leukemia,
Key Aspects of Peripheral Blood Films:
- Procedure: A drop of blood is placed on a slide, spread into a thin film, air-dried, fixed (usually with methanol), and stained (e.g., Wright-Giemsa) for examination.
- Microscopic Examination: A hematologist or technologist evaluates the cells for size, shape, color, and inclusions.
- Indications: Ordered to investigate abnormal Complete Blood Count (CBC) results, unexplained anemia, suspected leukemia, or infection.
- Common Findings:
- Red Blood Cells (RBCs): Evaluates for size (microcytic/macrocytic), shape (sickle cells, schistocytes, spherocytes), and color (hypochromic).
- White Blood Cells (WBCs): Assesses for leukocytosis, leukopenia, and differential counts (neutrophils, lymphocytes, etc.), including immature forms.
- Platelets: Estimates platelet count and morphology (giant platelets).
- Significance: It remains an indispensable, rapid, and low-cost tool for diagnosing hematological disorders, providing information that automated machines might miss, such as parasite detection (malaria) or specific, rare cell morphology.
এই সকল পরীক্ষা আধুনিক অটোমেটেড মেশিনের মাধ্যমে সম্পন্ন করা হয়, ফলে রিপোর্ট হয় নির্ভুল ও দ্রুত।
২. বায়োকেমিস্ট্রি বিভাগ
শরীরের বিভিন্ন অঙ্গের কার্যকারিতা নির্ণয়ের জন্য বায়োকেমিক্যাল পরীক্ষা অপরিহার্য।
আমাদের বায়োকেমিস্ট্রি টেস্টসমূহ:
Blood Sugar (Fasting, Random, 2 Hours After Meal)
Normal blood sugar (glucose) levels for non-diabetic adults are generally 70–100 mg/dL (3.9–5.6 mmol/L) when fasting, and less than 140 mg/dL (7.8 mmol/L) two hours after eating. Random blood sugar (at any time) usually remains

Normal Blood Sugar Levels (Non-Diabetic)
- Fasting (No food/caloric drinks for 8+ hours): 70–100 mg/dL (3.9–5.6 mmol/L).
- 2 Hours After Meal (Postprandial): Less than 140 mg/dL (7.8 mmol/L).
- Random (Any time): Typically 125 mg/dL or less. Levels up to 200 mg/dL may be acceptable, but
Key Considerations
- Prediabetes: Fasting 100–125 mg/dL; 2 hours post-meal 140–199 mg/dL.
- Diabetes: Fasting
mg/dL; 2 hours post-meal
mg/dL.
- Factors Affecting Levels: Stress, infections, illness, and medication can impact blood glucose levels.
- Symptoms of High Blood Sugar: Frequent thirst, urination, and blurred vision
HbA1c
HbA1c (glycated hemoglobin) is a blood test measuring average blood sugar levels over the past 2–3 months, used to diagnose and manage diabetes. It measures glucose attached to red blood cells, with results showing higher levels when blood sugar is poorly controlled. An HbA1c level of 48 mmol/mol (6.5%) or higher indicates diabetes.
Key HbA1c Information
- What it Measures: The percentage of hemoglobin coated with sugar (glycated).
- Significance: It reflects long-term glucose control, unlike daily, temporary finger-prick tests.
- Diagnosis Ranges:
- Normal: Below 42 mmol/mol (< 6.0%)
- Prediabetes: 42–47 mmol/mol (6.0%–6.4%)
- Diabetes: 48 mmol/mol or higher (≥ 6.5%)
- Targets for Diabetes Management:
- General Target: Below 53 mmol/mol (7%) for most adults.
- Strict Control: 48 mmol/mol (6.5%) or lower for some patients.
- Higher Target: 58–64 mmol/mol (7.5%-8%) for elderly or complex cases.
- Purpose: The test helps monitor, manage, and reduce the risk of long-term diabetes complications like kidney disease, blindness, and nerve issues.
Commonly Used Units
Results are commonly expressed in two ways:
- Percentage (%) – e.g., 6.5%
- Millimoles per mole (mmol/mol) – e.g., 48 mmol/mol
Test Frequency
People with diabetes should typically have their HbA1c checked every 3 to 6 months. No special preparation, such as fasting, is usually required.
Serum Creatinine
Serum creatinine is a waste product from muscle metabolism, measured in the blood to assess kidney function. Normal levels generally range from 0.7–1.3 mg/dL for men and 0.6–1.1 mg/dL for women, though these vary based on muscle mass, age, and gender. Elevated levels often indicate impaired renal function, such as chronic kidney disease (CKD) or acute injury, as the kidneys fail to filter it properly.
Key Aspects of Serum Creatinine
- Purpose: It is a key indicator used to estimate the glomerular filtration rate (eGFR), which measures how well the kidneys filter blood.
- Normal Ranges:
- Adult Men: 0.7 to 1.3 mg/dL (61.9 to 114.9 µmol/L).
- Adult Women: 0.6 to 1.1 mg/dL (53 to 97.2 µmol/L).
- Note: Ranges may vary slightly by laboratory.
- High Levels: A rise in serum creatinine indicates that the kidneys are not working at full capacity. Levels of 1.6–2.0 mg/dL or higher may suggest moderate to severe kidney dysfunction.
- Low Levels: These are less common but can be caused by low muscle mass, severe malnutrition, or certain liver diseases, though they are generally less alarming than high levels.
- Factors Influencing Results:
- Muscle Mass: Higher muscle mass usually means higher creatinine levels.
- Age: Older adults may have lower levels due to decreased muscle mass.
- Dehydration: Lack of fluids can temporarily increase serum creatinine levels.
- Diet: High meat consumption can temporarily raise levels.
Urea
A urea test, commonly known as a Blood Urea Nitrogen (BUN) test, measures the amount of urea nitrogen in the blood to evaluate kidney function and liver health. It checks for waste products produced by protein breakdown that are normally filtered by the kidneys. Normal levels for adults are generally 7 to 18 mg/dL or 2.5 to 7.8 mmol/L.
Key Details About the Urea Test
- Purpose: Evaluates kidney function, monitors for kidney disease, and checks for conditions like dehydration, heart failure, or high protein intake.
- Procedure: A blood sample is taken from a vein, typically in the arm.
- Preparation: Generally, no special preparation is required, but fasting may be necessary if combined with other tests.
- High Levels: Indicate potential kidney dysfunction, dehydration, heart failure, or high protein diet.
- Low Levels: Less common, but may indicate liver disease or malnutrition.
- Cost: Usually ranges from 400-500 taka.
Lipid Profile
A lipid profile is a blood test, usually requiring 10–14 hours of fasting, that measures fat levels—specifically total cholesterol, LDL (“bad”), HDL (“good”) cholesterol, and triglycerides—to assess cardiovascular health. It helps determine the risk of plaque buildup in arteries (atherosclerosis), which can
Components of a Lipid Profile
- LDL Cholesterol (Low-Density Lipoprotein): Known as “bad” cholesterol; high levels can build up in blood vessels.
- HDL Cholesterol (High-Density Lipoprotein): Known as “good” cholesterol; helps remove LDL from the bloodstream.
- Triglycerides: A type of fat from food; high levels increase risk.
- Total Cholesterol: The total sum of cholesterol in the blood.
- VLDL Cholesterol (Very Low-Density Lipoprotein): Moves triglycerides in the blood.
Typical Reference Ranges (May vary by lab)
- Total Cholesterol: Below 200 mg/dL (
).
- LDL Cholesterol: Less than 100 mg/dL (
for moderate risk).
- HDL Cholesterol: 40–60 mg/dL or higher (above 1.2 mmol/l for women, 1.0 mmol/l for men).
- Triglycerides: Below 150 mg/dL (
).
Purpose and Preparation
- Purpose: To evaluate risk for cardiovascular diseases, monitor treatment effectiveness, or screen for high cholesterol.
- Preparation: Usually requires fasting for 10-14 hours (water allowed).
- Risk: Minimal; includes potential, mild pain or bruising at the needle site.
SGPT (ALT)
Alanine aminotransferase (ALT), formerly known as Serum Glutamic-Pyruvic Transaminase (SGPT), is an enzyme found mainly in the liver. An ALT/SGPT blood test measures liver damage or inflammation, often detecting conditions like fatty liver, hepatitis, or cirrhosis by identifying leaked enzymes in the bloodstream.
Key Details About ALT/SGPT
- Purpose: Monitors liver health, screens for damage, and evaluates treatments for liver diseases.
- Normal Range: Typically between 7 and 56 U/L, though this varies slightly by laboratory.
- Elevated Levels: High levels generally indicate liver injury or inflammation.
- Causes of High Levels: Non-alcoholic fatty liver disease (NAFLD), alcohol-related damage, chronic hepatitis (B or C), and medication side effects.
- Preparation: Generally, no special preparation is required, but intense exercise 24-48 hours before the test should be avoided.
Symptoms Requiring an ALT Test
Doctors may order this test if you experience:
- Jaundice (yellowing of skin/eyes)
- Dark urine or light-colored stool
- Unexplained fatigue or weakness
- Abdominal pain, nausea, or vomiting
SGOT (AST)
AST (Aspartate Aminotransferase), also known as SGOT (Serum Glutamic-Oxaloacetic Transaminase), is an enzyme found in the liver, heart, muscles, and kidneys. A blood test measuring AST levels is primarily used to detect liver injury (such as hepatitis or cirrhosis) and, less frequently, heart or muscle damage, with normal ranges typically falling between 10–40 IU/L.
Key Aspects of AST (SGOT):
- Purpose: The test checks for liver damage or disease. It does not specifically measure how the liver is functioning, but rather if damage is occurring.
- Causes of High Levels: Elevated AST (SGOT) can indicate hepatitis, cirrhosis, fatty liver, liver infection, or damage to other organs like the heart.
- Symptoms of High Levels: Potential signs include jaundice (yellowing skin/eyes), fatigue, abdominal pain, nausea, and dark urine.
- Normal Range: Generally 10–40 units/L for males and 9–32 units/L for females, though ranges vary by lab.
Bilirubin
Bilirubin is a yellow-orange pigment formed from the natural breakdown of red blood cells (hemoglobin). Processed by the liver and excreted in bile, it acts as an antioxidant but causes jaundice (yellowing of skin/eyes) if levels are too high. High bilirubin (typically

) often signals liver, gallbladder, or blood disorders.
Key Aspects of Bilirubin
- Production: Roughly 80% comes from hemoglobin in old red blood cells; the rest comes from other heme-containing proteins.
- Types:
- Unconjugated (Indirect): Fat-soluble, travels from blood to the liver. High levels indicate increased red cell destruction (hemolysis) or genetic conditions like Gilbert’s syndrome.
- Conjugated (Direct): Water-soluble, processed by the liver for excretion. High levels indicate liver dysfunction (hepatitis, cirrhosis) or bile duct obstructions.
- Total Bilirubin: The sum of both types.
- Normal Ranges (Adults): Generally
for total bilirubin, with direct being
.
- Significance: It is used in liver function tests to diagnose jaundice, gallbladder disease, or hemolytic anemia.
Causes of Elevated Levels (Hyperbilirubinemia)
- Liver Dysfunction: Hepatitis, cirrhosis, or liver cancer.
- Biliary Issues: Gallstones or bile duct obstructions.
- Hemolysis: Excessive breakdown of red blood cells.
- Newborns: High levels are common due to immature liver function, which can be toxic to the brain if not monitored.
Total Protein
Total protein is a blood test measuring the combined amount of albumin and globulin, which are essential for immune function, tissue growth, and fluid balance. Typically ranging from 6.0 to 8.3 g/dL (or 60–80 g/L), it helps evaluate liver or kidney disease and nutritional status. High levels may indicate dehydration or chronic inflammation, while low levels suggest liver/kidney disorders or malnutrition.
Key Aspects of Total Protein
- Components: The test measures two major proteins: Albumin (maintains fluid balance, transports substances) and Globulin (immune system, liver health).
- Normal Range: While 6.0 to 8.3 g/dL is common, reference ranges vary by laboratory.
- Low Levels (Hypoproteinemia): Possible causes include liver disease, kidney disease (protein loss), malnutrition, or malabsorption conditions like celiac disease.
- High Levels (Hyperproteinemia): Often caused by dehydration, or serious conditions like bone marrow disorders (multiple myeloma), chronic infection, or inflammation.
- Why it’s tested: Used to assess overall nutritional health, check for kidney or liver dysfunction, or investigate symptoms like fatigue or unexplained weight loss.
Factors Affecting Levels
- Dehydration: The most common cause of falsely high total protein.
- Diet: Adequate protein intake ensures proper synthesis.
- Medical Conditions: Chronic liver disease, kidney dysfunction, or immune system disorders significantly alter these protein levels.
Albumin Test
An albumin test measures the level of albumin, a protein produced by the liver, in the blood or urine to assess liver and kidney function. It is used to detect liver disease, kidney disease, or malnutrition, with normal serum levels typically ranging from 3.4 to 5.4 g/dL. Low levels may indicate liver/kidney damage, while high levels often signal dehydration.
Key Details About the Albumin Test:
- Purpose: The test evaluates how well the liver and kidneys are functioning, checks nutritional status, and helps diagnose chronic diseases.
- What it Measures: Serum albumin checks the protein levels in the blood, while a urine albumin test (often with a creatinine ratio) checks for leakage from the kidneys.
- Normal Results: A typical range for serum albumin is 3.4 to 5.4 g/dL (34 to 54 g/L), though this can vary slightly by lab.
- Low Albumin (Hypoalbuminemia): Indicates potential issues like liver disease (cirrhosis), kidney disease (nephrotic syndrome), malnutrition, or inflammatory conditions.
- High Albumin (Hyperalbuminemia): Usually indicates dehydration.
- Procedure: A blood sample is taken from a vein in the arm. No fasting is typically required, but instructions should be followed.
Why the Test is Performed
- Liver Diseases: To check for cirrhosis or liver damage, as the liver produces albumin.
- Kidney Disease: To see if kidneys are allowing protein to leak into urine.
- Nutritional Status: To monitor severe malnutrition or malabsorption.
- Symptoms: Used if you have jaundice, fatigue, weight loss, or abdominal swelling (edema).
সরকার নির্ধারিত মূল্যে এই পরীক্ষাগুলো সম্পন্ন করা হয়, যাতে ডায়াবেটিস, লিভার রোগ, কিডনি সমস্যা ইত্যাদি দ্রুত শনাক্ত করা যায়।
৩. ইমিউনোলজি ও সিরোলজি বিভাগ
সংক্রমণ ও ভাইরাসজনিত রোগ নির্ণয়ে এই বিভাগ অত্যন্ত গুরুত্বপূর্ণ।
আমাদের পরীক্ষাসমূহ:
HBsAg
HBsAg (Hepatitis B surface antigen) is a protein on the surface of the Hepatitis B virus, and its presence in a blood test indicates an acute or chronic Hepatitis B infection, meaning the person is contagious. A positive HBsAg result warrants further testing for diagnosis, as it signifies HBV infection and potential liver risk. Hepatitis B Foundation +4
Key Aspects of HBsAg Testing
- Purpose: Detects active hepatitis B virus (HBV) infection, which can lead to cirrhosis or liver cancer.
- Positive Result (+): Indicates current infection, and the person can transmit the virus through blood or body fluids.
- Negative Result (-): Indicates the absence of an active infection.
- Types of Infections: Detected during both acute (recent) and chronic (long-term) infections.
- Screening: Recommended for pregnant women, healthcare workers, and those with high-risk behaviors (e.g., shared needles, multiple partners).
Hepatitis B Foundation +4
Clinical Significance & Further Tests
- HBsAb/Anti-HBs (Surface Antibody): Indicates immunity from vaccination or past infection.
- HBcAb (Core Antibody): Indicates previous or ongoing infection.
- Management: While 95% of adults recover from acute infection, HBsAg persistence >6 months signals chronic infection, requiring, in some cases, antiviral treatment to control viral load
Anti-HCV
The Anti-HCV test detects antibodies produced by the immune system to fight the Hepatitis C virus, indicating past or present exposure to the virus. A positive result means exposure, not necessarily an active infection, requiring further testing (HCV RNA PCR) to confirm if the virus is currently present.
Key Details About Anti-HCV
- Purpose: Screens for exposure to Hepatitis C, a virus that causes liver inflammation.
- Interpretation:
- Reactive (Positive): Indicates previous exposure. About 15-25% of people clear the virus on their own, meaning a positive antibody test doesn’t always mean active infection.
- Non-reactive (Negative): No antibodies detected, typically indicating no infection.
- Next Steps: If reactive, an HCV RNA test is necessary to determine if there is an active infection.
- Timing: Antibodies may take 6-10 weeks to develop after exposure (the “serologic gap”).
- Transmission: Spread through contact with infected blood, often via shared needles or contaminated medical equipment.
- Treatment: Modern treatments are highly effective, with cure rates exceeding 95%
HIV Screening
HIV screening involves blood or oral fluid tests that detect HIV antibodies, antigens (like p24), or the virus’s genetic material (RNA) to identify infection. The CDC recommends all individuals aged 13-65 get tested at least once, with high-risk individuals screened every 3-6 months. Common tests include 4th-generation antigen/antibody tests, which are highly accurate 18-45 days after exposure. Centers for Disease Control and Prevention | CDC (.gov) +5
Types of HIV Tests
- Antigen/Antibody Tests (Lab): Most common. These tests use blood from a vein and can detect HIV 18-45 days after exposure.
- Rapid Antibody/Antigen Tests: Finger-prick blood tests that provide results in 20-30 minutes.
- Nucleic Acid Tests (NAT): Detects the virus directly, often 10-33 days after exposure, but primarily used to monitor treatment or confirm high-risk cases.
- Self-Tests: FDA-approved rapid kits, often using oral fluid or a finger prick, allow for private testing.
When to Get Tested (Window Period)
The “window period” is the time between exposure and when a test can accurately detect the virus.
- Antigen/Antibody (Lab): 18–45 days post-exposure.
- Rapid/Self-Test (Antibody): 23–90 days post-exposure.
Why Screen?
- Early Diagnosis: Enables immediate treatment, which significantly reduces morbidity and mortality.
- Prevention: Knowing your status allows for immediate antiretroviral therapy (ART), preventing transmission to partners.
- Routine Health: Recommended for all, but crucial for those with high-risk behaviors, such as unprotected sex or sharing needles.
Widal Test
The Widal test is a serological blood test used to diagnose typhoid and paratyphoid fever, caused by Salmonella bacteria, by detecting specific antibodies (agglutinins) against O (somatic) and H (flagellar) antigens. It is commonly used in developing regions due to its low cost and simplicity. Wikipedia +2
Key Aspects of the Widal Test
- Purpose: Detects antibodies (IgM and IgG) that develop against S. typhi and S. paratyphi.
- Timing: The test is most accurate when conducted after the first week of fever (around 7-14 days), as it requires time for antibodies to build up.
- Procedure: A blood sample is taken, and serum is mixed with bacterial suspensions (O and H antigens). Agglutination (clumping) indicates a positive result.
- Results Interpretation: Results are given as a “titre” (e.g., 1:80, 1:160).
- Normal: Usually
or
.
- Positive: A high or rising titre, generally
or
, suggests infection.
- Normal: Usually
- Limitations: The Widal test has low specificity and can yield false-positive results due to prior vaccination, past infection, or other infections like malaria.
- Alternative Tests: Typhidot and blood cultures are often used for more accurate diagnosis.
CRP
C-Reactive Protein (CRP) is a protein produced by the liver that rises in the blood in response to inflammation. A CRP blood test acts as a general, non-specific indicator of inflammation, infection, or tissue injury. It is used to detect acute infections, monitor chronic inflammatory conditions (like arthritis),
Key Facts About CRP:
- Normal Levels: Generally, a healthy person has low levels (0–0.5 mg/L or 0.8–3.0 mg/L depending on the lab), with higher levels indicating potential issues.
- High Levels: Significant elevation (e.g., >50 mg/L) often points to severe, acute infection, or acute injury.
- Conditions Detected: High CRP can indicate bacterial infections, autoimmune diseases (lupus, rheumatoid arthritis), inflammatory bowel disease, or damage to tissues.
- Heart Risk: A specific high-sensitivity test (hs-CRP) is used to estimate the risk of heart attacks.
RA Test
The RA (Rheumatoid Factor) test is a blood test that measures antibodies to help diagnose rheumatoid arthritis (RA) and other autoimmune conditions, such as Sjögren’s syndrome. It identifies high levels of RF, which indicates the immune system is mistakenly attacking healthy tissues. A positive result, usually over

Key Aspects of the RA Test
- Purpose: The test helps doctors diagnose RA, assess disease severity, and differentiate it from other types of arthritis.
- Procedure: It is a simple blood sample collection, often taken alongside other tests like ESR or CRP to check for inflammation.
- Preparation: No special fasting is required in most cases, but you should inform your doctor about all medications and supplements.
- Results: A normal result is usually less than
.
- Positive: Suggests the presence of autoimmune disease, most commonly rheumatoid arthritis.
- Negative: Suggests the absence of RF, though some individuals with RA may test negative (“seronegative RA”).
- Limitations: A positive result alone cannot confirm RA, as elevated levels can occur due to other chronic infections or autoimmune conditions.
Yashoda Hospitals +7
Related Diagnostic Tests
Doctors may combine the RA test with other tests for a more accurate diagnosis:
- Anti-CCP (Anti-cyclic citrullinated peptide): More specific to RA than the RA factor.
- ESR (Erythrocyte Sedimentation Rate): Measures general inflammation.
- CRP (C-reactive protein):
ASO Titre
An ASO (Anti-Streptolysin O) Titre is a blood test measuring antibodies against toxins produced by Group A Streptococcus bacteria, indicating a recent strep infection. It diagnoses post-streptococcal complications like rheumatic fever or glomerulonephritis. Normal levels are typically
Key Details About ASO Titre Test:
- Purpose: Identifies if previous, untreated, or inadequately treated strep infections (e.g., strep throat, scarlet fever) have caused secondary illnesses.
- Elevated Results: High levels suggest a recent streptococcal infection. A second test 10–14 days later may be done to see if levels are rising (active infection) or falling (recovering).
- Symptoms Prompting Test: Fever, joint pain/swelling, skin rash, or decreased, bloody, or foamy urine.
- Procedure: A standard blood sample is taken, usually with minimal risk.
- Limitations: ASO levels may not rise in all streptococcal skin infections (like pyoderma)
Dengue NS1
The Dengue NS1 (Nonstructural Protein 1) antigen test is a rapid diagnostic tool used to detect acute dengue infection within the first 1–7 (up to 9) days of fever. It is highly effective for early diagnosis, often before antibodies (IgM) appear. A positive NS1 result confirms infection, requiring immediate clinical
Key Details About Dengue NS1
- What it Detects: The NS1 test detects a glycoprotein (NS1) secreted into the blood by the dengue virus during the acute, viremic phase of the infection.
- Optimal Timing: Testing is most effective from day 1 to day 7 after symptom onset.
- Significance of Results:
- Positive: Indicates an active, acute dengue infection.
- Negative: Does not completely rule out dengue, especially if symptoms have lasted more than 7 days, as the antigen levels may have decreased.
- Advantages: The test allows for early diagnosis and intervention, which is crucial for preventing severe dengue complications like dengue hemorrhagic fever or dengue shock syndrome.
- Comparison to Other Tests: While NS1 is ideal for early detection (days 1-7), IgM antibody tests are Control and Prevention
Next Steps After Positive Result
If the NS1 test is positive, it is important to consult a healthcare provider immediately, as management typically involves:
- Monitoring: Frequent checks on platelet count and hematocrit levels.
- Hydration: Increasing fluid intake (water, coconut water, or oral rehydration solutions) to manage high fever and dehydration.
- Medication: Avoiding aspirin and ibuprofen, which can increase bleeding risk; acetaminophen is generally used for fever.
Typhoid Test
Typhoid fever is diagnosed through laboratory tests that detect Salmonella typhi bacteria or antibodies in blood, stool, urine, or bone marrow. The “gold standard” is a blood culture, while common, faster, but less accurate methods include the Widal test (antibody detection) and rapid IgG/IgM tests like Typhidot.
- Blood Culture: The preferred diagnostic method, especially in the first week of fever, to detect live bacteria.
- Widal Test: A, serology test that identifies antibodies (O and H antigens) against Salmonella bacteria. It is common in low-resource settings but can be unreliable and show false positives.
- Typhidot/Rapid IgM/IgG Test: An ELISA-based test that detects specific IgM (early infection) and IgG (past infection) antibodies, usually within 2–3 days of infection.
- Stool/Urine Culture: Detects the bacteria in body fluids, often used to confirm the infection or check
Test Results Interpretation
- Positive: Presence of IgM/IgG antibodies (Typhidot) or specific titers (Widal) indicate recent or current infection.
- Negative: No antibodies or bacteria detected, though false negatives can occur early in the infection.
Important Considerations
- Timing: Blood cultures are most effective in the first week, while antibody tests (Widal) are usually more reliable after the first week of symptoms.
- Preparation: Generally, no fasting is required for typhoid tests.
- Limitations: Widal tests can cross-react with other infections, causing false positives.
- Accuracy: Rapid tests (like Typhidot) are generally more sensitive and specific than the traditional Widal test.
সকল পরীক্ষাই মানসম্মত কিট ব্যবহার করে সম্পন্ন করা হয়।
৪. ইউরিন ও স্টুল পরীক্ষা
Urine R/E
A Urine Routine Examination (Urine R/E or R/M) is a common, non-invasive lab test that analyzes urine to check for diseases like UTIs, kidney dysfunction, liver issues, and diabetes. It involves checking the urine’s physical appearance (color, clarity), chemical properties (pH, protein, glucose), and microscopic
Key Aspects of a Urine R/E Test:
- Physical Exam: Checks for color (normally yellow) and clarity (cloudy urine may indicate infection or protein).
- Chemical Exam (Dipstick): Measures pH (acidity), specific gravity (concentration), protein (kidney function), glucose (diabetes), bilirubin/urobilinogen (liver), and nitrites/leukocytes (infection).
- Microscopic Exam: Analyzes sediment for red blood cells (blood), white blood cells
Common Reasons for Testing:
- Routine Health Screening: Part of annual checkups.
- Symptoms: Back/abdominal pain, frequent/painful urination, cloudy/bloody urine.
- Pre-surgery Checkup: To ensure kidney function.
Preparation and Results:
- A clean-catch, mid-stream urine sample is typically required.
- Results are usually available quickly, often within a few hours to a day.
- Positive Culture: If a Urine R/E suggests infection, a follow-up “Urine Culture and Sensitivity” (Urine C/S) is often required to identify the specific bacteria and the right antibiotic.
Urine C/S
Stool R/E
Stool Occult Blood
এই পরীক্ষাগুলো কিডনি, মূত্রনালী ও পরিপাকতন্ত্রের সমস্যা নির্ণয়ে সহায়ক।
৫. হরমোন টেস্ট
হরমোনজনিত সমস্যার সঠিক নির্ণয়ের জন্য:
- TSH
- T3
- T4
- LH
- FSH
- Prolactin
সরকার নির্ধারিত মূল্যে হরমোন টেস্ট করা হয়।
আধুনিক প্রযুক্তি ও দক্ষ জনবল
HRTD Medical Institute-এ ব্যবহৃত হয় আধুনিক ও মানসম্পন্ন ল্যাবরেটরি যন্ত্রপাতি। আমাদের দক্ষ মেডিকেল টেকনোলজিস্ট ও প্যাথলজি বিশেষজ্ঞরা প্রতিটি রিপোর্ট যথাযথভাবে যাচাই করেন।
আমরা নিশ্চিত করি:
- সঠিক স্যাম্পল সংগ্রহ
- যথাযথ সংরক্ষণ
- মান নিয়ন্ত্রণ ব্যবস্থা
- নির্ভুল রিপোর্ট প্রদান
দ্রুত রিপোর্ট সরবরাহ
সময়মতো রিপোর্ট পাওয়া চিকিৎসার জন্য অত্যন্ত গুরুত্বপূর্ণ। আমাদের প্রতিষ্ঠানে অধিকাংশ টেস্টের রিপোর্ট একই দিনে প্রদান করা হয়। প্রয়োজনে জরুরি রিপোর্ট দ্রুত সরবরাহ করা হয়।
রোগীবান্ধব পরিবেশ
আমাদের প্রতিষ্ঠানটি পরিচ্ছন্ন, সুশৃঙ্খল এবং নিরাপদ পরিবেশে পরিচালিত হয়। রোগীদের আরাম ও গোপনীয়তা রক্ষা করা আমাদের অগ্রাধিকার।
কেন HRTD Medical Institute নির্বাচন করবেন?
✔ সরকার নির্ধারিত মূল্য
✔ নির্ভুল রিপোর্ট
✔ আধুনিক যন্ত্রপাতি
✔ দক্ষ জনবল
✔ সহজ যোগাযোগ ব্যবস্থা
✔ নির্ভরযোগ্য সেবা
সামাজিক দায়বদ্ধতা
HRTD Medical Institute শুধু একটি ডায়াগনস্টিক সেন্টার নয়—এটি একটি সামাজিক উদ্যোগ। আমরা বিশ্বাস করি, সবার জন্য স্বাস্থ্যসেবা নিশ্চিত করাই আমাদের প্রধান দায়িত্ব।
সরকার নির্ধারিত মূল্যে টেস্ট করার মাধ্যমে আমরা সমাজের প্রতিটি স্তরের মানুষকে স্বাস্থ্যসেবা গ্রহণে উৎসাহিত করি।
উপসংহার
স্বাস্থ্যই সম্পদ। সঠিক রোগ নির্ণয় ছাড়া সঠিক চিকিৎসা সম্ভব নয়। তাই নির্ভুল, দ্রুত এবং সরকার নির্ধারিত মূল্যে প্যাথলজিক্যাল টেস্ট অত্যন্ত গুরুত্বপূর্ণ।
HRTD Medical Institute গর্বের সাথে ঘোষণা করছে যে, আমরা সরকার নির্ধারিত মূল্যে সকল ধরনের প্যাথলজিক্যাল টেস্ট প্রদান করে থাকি। আমাদের লক্ষ্য হলো মানসম্মত ও সাশ্রয়ী স্বাস্থ্যসেবা নিশ্চিত করা।
আপনার ও আপনার পরিবারের সুস্থতার জন্য আজই যোগাযোগ করুন:
HRTD Medical Institute
Section-6, Block-Kha, Road-1, Plot-11
Metro Rail Pillar-249
Folpotti Mosque Lane
Mirpur-10, Dhaka-1216
📞 01797522136
📞 01987073965
📞 01784572173
স্বল্প খরচে, নির্ভুল রিপোর্ট, বিশ্বস্ত সেবা—এটাই আমাদের প্রতিশ্রুতি।
 Pathology Training Institute in Bangladesh Best Pathology Training Institute in Bangladesh
Pathology Training Institute in Bangladesh Best Pathology Training Institute in Bangladesh